Dental implants are commonly described as a “permanent” solution, but permanent is a term worth examining. The short answer is that the titanium post component of an implant can last 20 to 30 years, and many last longer than that. The longer answer is that longevity depends significantly on factors within and outside your control.
Dental implants are designed to function as a long-term tooth replacement for missing teeth, but like any treatment, outcomes vary from patient to patient. As a surgical or invasive procedure, implant treatment carries risks, and this information should be discussed with an appropriately qualified health practitioner before you proceed.
Understanding what drives long-term implant success, and what affects implant longevity, is useful both for patients weighing whether to proceed and for those who already have implants and want to protect them.
Key Takeaways
- The titanium implant post has a long-term survival rate of approximately 95% at 10 years; many function well for 20-30 years or longer
- The crown attached to the implant typically lasts 10-20 years and may require replacement before the post does
- Peri-implantitis, a bacterial infection of the tissue surrounding the implant, is the primary cause of late implant failure and is largely preventable with consistent oral hygiene
- Smoking significantly increases implant failure risk; complication rates in smokers are substantially higher than in non-smokers
- Regular professional hygiene appointments and periodic implant monitoring are essential throughout the life of the implant, not just in the initial healing period
The Implant Post vs the Crown: Two Different Lifespans
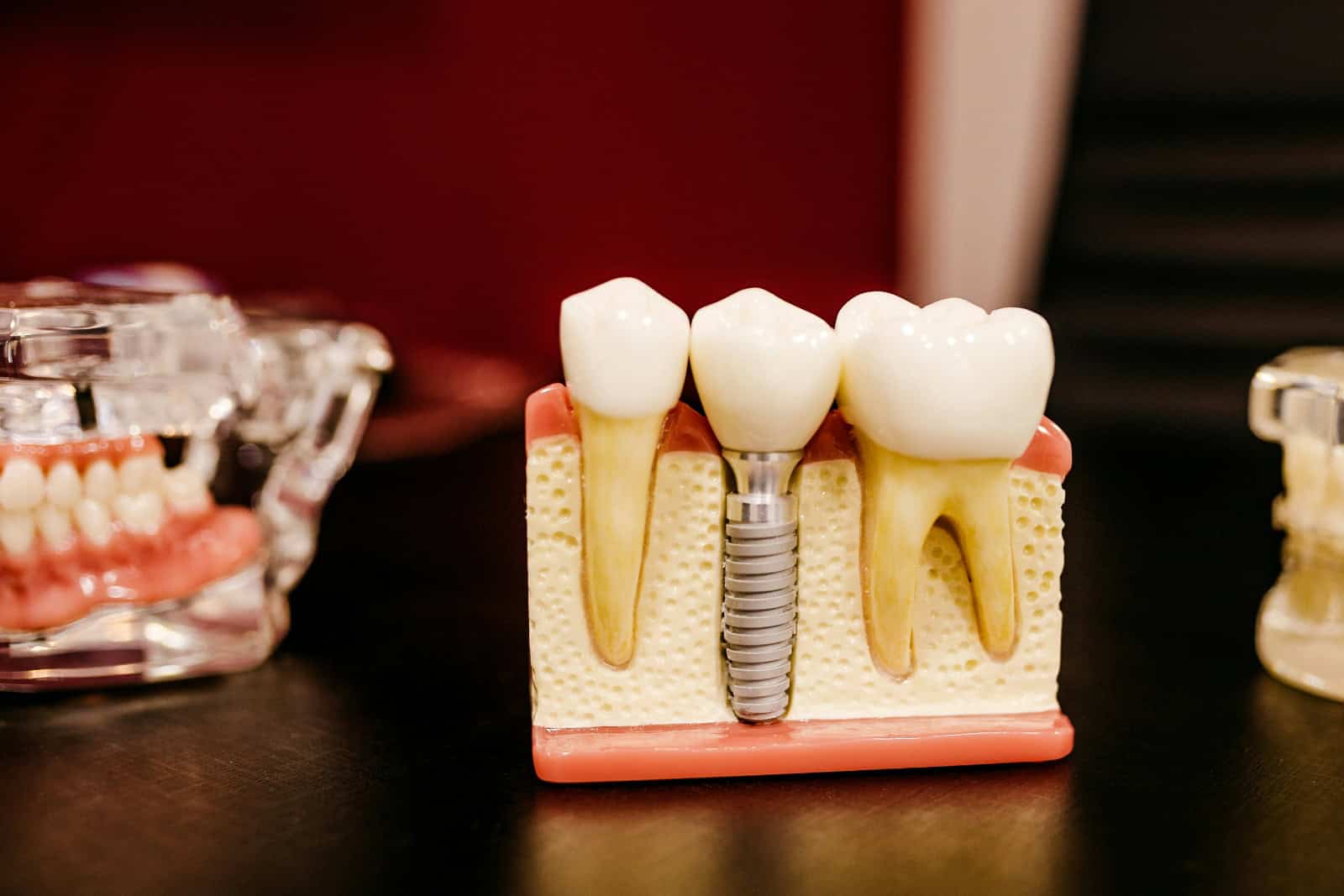
A dental implant has two distinct components with different longevity profiles, and it helps to understand them separately.
The titanium post, the artificial tooth root surgically placed into the jaw bone, is the most durable component. Once the process called osseointegration is complete and the post is stable within the bone, it can remain in place for decades without issue. Published research consistently shows a success rate of approximately 95% at 10 years, and many implants placed 20 to 30 years ago continue to function well today.
The dental crown, the visible, functional tooth attached to the post via an abutment, is subject to chewing forces, wear, and the same mechanical stresses that affect natural teeth. Crowns typically last 10-20 years before they may require replacement, though high quality crowns made from modern materials fare better. Zirconia crowns are generally more wear-resistant than older porcelain-fused-to-metal options, though all crown materials have a finite lifespan under normal use.
What this means in practice: patients who receive an implant in their 50s or 60s may need a crown replacement once but will often keep the post for life. Patients who receive implants in their 30s or 40s are more likely to need the crown replaced at some point, but the titanium post beneath may continue functioning indefinitely with proper care.
What Affects How Long an Implant Lasts?
Several factors influence the lifespan of dental implants. Some are within your control; others relate to your medical history and overall health.
Oral Hygiene
The single most important factor for long-term implant success is oral hygiene, specifically, keeping the tissue and bone around the implant free from bacterial accumulation.
Dental implants cannot develop cavities, but the tissue surrounding them is vulnerable to the same bacterial activity that causes gum disease around natural teeth. Poor oral hygiene leads to plaque buildup around the implant site, which is the primary driver of peri-implantitis, an inflammatory condition that often progresses faster than conventional gum disease and, critically, with less pain. This means it can advance significantly before a patient notices anything is wrong.
Left untreated, peri-implantitis causes progressive bone loss around the implant. As the supporting bone recedes, the implant loses its foundation and can ultimately fail. This is the leading cause of late implant failure, and it is largely preventable by practising good oral hygiene consistently.
Effective daily cleaning for implants includes:
- Brushing with a soft-bristle toothbrush, twice daily, paying attention to the gum line around the implant
- Interdental cleaning, flossing, interdental brushes, or a water flosser, specifically around the implant and abutment
- Using any specific cleaning aids recommended by your dentist for your implant configuration
Technique matters as much as the tools. Your dentist and hygienist can advise on the most effective approach for your specific implant position and restoration type.
Professional Hygiene Appointments
Even with good oral hygiene at home, professional hygiene appointments are essential for implant longevity. A hygienist can remove calculus and build-up from implant surfaces and surrounding tissue that brushing cannot reach, and can assess the health of the gum and bone around the implant at each visit. Early detection of changes to the surrounding bone allows problems to be managed before they become significant.
Regular dental check-ups every six months are a minimum for patients with implants. Some patients benefit from more frequent visits depending on their individual risk profile, patients who grind, smoke, or have a history of gum disease may require quarterly appointments to stay ahead of potential problems.
These appointments should not be treated as optional once the implant has settled in. Peri-implantitis can develop years after an implant is placed, and seeing your dentist regularly is the most reliable way to catch early changes before they require more involved treatment.
Smoking
Smoking is one of the most significant risk factors for implant failure. It reduces blood flow to healing tissue, suppresses the immune system’s response to bacteria, and creates an oral environment more prone to infection, all of which affect both the initial healing process and the long-term oral health of the tissue surrounding an established implant.
Research consistently shows that smokers have substantially higher implant failure and complication rates than non-smokers at every stage of implant surgery and beyond. Estimates vary across studies, but complication rates in smokers are commonly reported at two to three times those in non-smokers, and failure rates are meaningfully elevated at every time point measured.
If you smoke and are considering implants, avoiding smoking before and after implant surgery is one of the most impactful steps you can take. Ceasing smoking, or at minimum substantially reducing, before and after the procedure improves outcomes significantly.
Systemic Health Conditions
Certain health conditions and lifestyle habits affect how bone heals and how well it maintains the implant over time:
- Diabetes: uncontrolled diabetes impairs healing and increases infection susceptibility. Well-controlled diabetes is not an automatic barrier to implants, but it requires careful management and closer follow-up than for patients without the condition
- Osteoporosis and bone density concerns: can affect the quality of bone available to support the implant; assessment is required before treatment decisions are made. Bone health is an important consideration at the treatment planning stage
- Medications affecting bone: bisphosphonates (used for osteoporosis treatment) and some cancer therapies carry specific implications for implant candidacy and healing; this should be discussed with both the treating dentist and the prescribing specialist before proceeding
- Excessive alcohol consumption: heavy alcohol use impairs healing and is associated with higher risk of post-surgical complications and peri-implantitis
Most medical conditions do not automatically rule out implant treatment. They require careful pre-treatment assessment and, in some cases, specialist medical clearance, but many patients with managed health conditions have successful implant outcomes.
Bone Grafting and Bone Quality
Some patients require bone grafting before implant placement if there is insufficient bone volume to support the implant post. The quality and quantity of bone available at the implant site, and the success of any preparatory bone grafting, directly affects how well the implant integrates and how stable it remains over the long term. Your dentist or specialist will assess bone quality through imaging before treatment planning begins.
Bruxism (Teeth Grinding)
Patients who grind or clench their teeth place significantly higher mechanical loads on implants and crowns than non-grinders. Unmanaged bruxism can crack or fracture crowns, stress the abutment connections, and, in severe cases, affect the interface between the implant and the bone. Excessive force over time can lead to implant failure even when everything else is managed well.
If you grind, a custom-fitted occlusal splint (night guard) worn during sleep is an important protective measure after implant treatment. This is worth raising at the treatment planning stage, before placement. An over-the-counter guard is not an adequate substitute, a custom-fitted splint from your dentist distributes forces correctly and protects both the implant and the surrounding teeth.
Location of the Implant
Posterior (back) teeth experience higher bite forces than anterior (front) teeth. Well-placed posterior implants have excellent long-term outcomes, but the mechanical demands are greater, crown wear and fracture risk is higher in these positions, and crown material selection is particularly important. Your dentist can advise on the most durable crown option for the specific site.
Quality of Placement and Restoration
Implant placement by a skilled dentist with specific implant training is one of the foundations of long-term success. Accurate positioning of the post, in terms of depth, angle, and proximity to adjacent teeth, nerves, and the sinus, determines the mechanical loads the implant experiences and how easily the patient can clean around it. Poorly positioned implants are harder to maintain and more prone to peri-implantitis.
A balanced diet that supports bone health and tissue healing also contributes to the long-term stability of the implant, particularly in the months following implant surgery.
The quality of the final restoration also affects long-term outcomes. A well-fitted final restoration with correctly calibrated bite alignment distributes chewing forces evenly; a poorly fitted one creates stress concentrations that accelerate wear on both the crown and the post-abutment connection.
Early vs Late Implant Failure
Implant failures fall broadly into two categories with different causes and different solutions.
Early failure occurs within the first few months, during or shortly after the osseointegration period. The most common cause is failure of the post to fuse with the jaw bone. Risk factors include insufficient bone volume, poor bone density, infection during the healing phase, and premature loading before osseointegration is complete. Early failure rates are low, typically 2-5% in healthy patients, but they do occur.
If early failure happens, the failed implant is removed, the site is allowed to heal, and in most cases a new implant can be placed after a waiting period. Early failure is not the end of the road, and most patients who experience it go on to have a successful outcome with a second attempt. Patients who have concerns about their outcome are entitled to seek a second opinion from another appropriately qualified health practitioner.
Late failure occurs after osseointegration is complete, months or years after the implant is established and functioning. Peri-implantitis is the primary driver of late failure. Trauma, excessive mechanical loading from unmanaged bruxism, and hardware complications (rarely, the metal post itself fracturing) account for a smaller proportion of late failures.
The distinction matters because early and late failures have different causes, different presentations, and different remediation paths. Your dentist or specialist will identify the mechanism and advise accordingly.
How to Protect Your Implant Long-Term
The measures most likely to protect a long-term implant investment:
- Daily cleaning: brush twice a day, clean interdentally around the implant with floss, interdental brushes, or a water flosser; focus on the gum line where bacteria accumulate
- Regular dental visits: professional hygiene appointments at minimum every six months; do not let these lapse once the implant is established
- Periodic implant monitoring: regular X-rays allow your dentist to check bone levels around the implant and detect early bone loss before it becomes clinically significant; early detection matters
- Night guard if you grind: custom-fitted, worn consistently during sleep
- Avoid using your implant as a tool: opening packaging, biting hard foods, or habits like chewing ice increase crown fracture risk
- Address problems promptly: pain, movement, swelling, or a change in how the implant feels when biting should be assessed without delay
Signs Something May Be Wrong
Not all implant problems announce themselves clearly. Warning signs to take seriously include:
- Pain or discomfort around the implant that is new or increasing
- Swelling, redness, or bleeding at the gum margin around the implant site
- Any perceptible movement in the implant or its crown
- A change in bite feel, the implant feeling higher or lower when you close
- Persistent bad taste or odour localised to the implant area
Peri-implantitis in particular can be relatively painless in its early stages. By the time pain is obvious, significant bone loss may have already occurred. This is one of the strongest arguments for regular professional monitoring even when nothing subjectively feels wrong.
If any of these signs are present, contact your dental practice promptly rather than waiting for the next scheduled appointment.
How Implant Longevity Compares to the Alternatives
When longevity is included in the comparison, implants hold up well against other tooth replacement options:
Dental bridges, the most common fixed alternative for a single missing tooth, typically last 10-15 years before failure of a support crown or a change in the health of the anchor teeth. Bridges require grinding down adjacent healthy teeth to serve as supports, and those surrounding teeth may develop complications over time. The bridge’s lifespan is contingent on the ongoing health of the teeth it relies on.
Dentures require relining every five to seven years as the jaw changes shape, and full replacement approximately every decade. Bone loss beneath the denture continues throughout its life, a structural consequence that, over years, affects facial appearance, fit, and the stability of any remaining natural teeth.
Dental implants, by contrast, actively preserve jaw bone by transmitting chewing forces into it, the same stimulus that healthy natural tooth roots provide. This bone-preservation effect compounds over time and represents a structural benefit that other tooth replacement options cannot replicate. For patients who are suitable candidates, implants provide a solid foundation for long-term oral health.
See our guide on dental implants vs dentures and the dental implants cost breakdown for a broader comparison of the long-term clinical and financial case for each option.
Frequently Asked Questions
Do dental implants last forever?
No implant is guaranteed to last indefinitely. “Permanent” in this context means the post fuses with the jaw bone and functions under normal conditions without replacement, not that no future monitoring is needed. For many patients the post does function for life; the crown is the component more likely to need attention over time.
Can a dental implant fall out?
An osseointegrated implant does not fall out spontaneously under normal circumstances. Movement or loosening signals that something has gone wrong, most commonly peri-implantitis causing bone loss, or a problem with the abutment connection. A loose crown is more common and usually simpler to resolve. Any movement, in the post or the crown, should be assessed promptly.
Can I have an MRI with dental implants?
Yes. Dental implants are made of titanium, which is non-magnetic and considered MRI-safe. Implants do not need to be removed before a scan. The metal can occasionally cause minor image artefacts on scans of the head or jaw, so let the radiographer know about your implants before the appointment.
Is there a warranty on dental implants?
Some implant manufacturers provide warranties on the hardware (post, abutment, and associated fixings) covering manufacturing defects. Your dental practice can confirm what applies to the specific implant system used in your treatment. Hardware warranties cover component defects, not biological outcomes such as peri-implantitis or osseointegration failure.
Long-Term Implant Care at Our Balwyn Practice
Implant aftercare is built into the treatment plan at our Balwyn practice from the outset, not treated as an afterthought once the restoration is fitted. Dr Rostkier provides specific cleaning instructions for each patient’s implant configuration after the final crown or prosthesis is placed. Our dedicated hygiene department, one of Victoria’s longest-running, operating for nearly 30 years, provides professional implant maintenance appointments to monitor the health of surrounding tissue and bone over time.
For patients with existing implants placed elsewhere who are seeking ongoing monitoring and hygiene care, we’re able to help. Understanding the history of the implant and assessing its current status through clinical examination and updated imaging gives us the foundation to look after it going forward.
To book a check-up or implant hygiene appointment, call (03) 9831 3272 or book your appointment online now. We see patients from Balwyn, Balwyn North, Deepdene, Canterbury, Camberwell, Hawthorn, Box Hill, Surrey Hills, Mont Albert, Kew, and Doncaster.
Any surgical or invasive procedure carries risks. Before proceeding with dental implant treatment, seek a second opinion from an appropriately qualified health practitioner. Dr Steven Rostkier BDSc (University of Melbourne, 1999) has 25+ years of clinical experience in general and restorative dentistry, with a focus on implant-supported restorations and complex full-arch rehabilitation. He practises at 2a/379-381 Whitehorse Rd, Balwyn VIC 3103. This content is for general information only and does not constitute clinical advice. Individual outcomes depend on assessment findings specific to each patient.